Geneva Surgery
Geneva Surgery
CHOLECYSTECTOMY
CHOLECYSTECTOMY
The following answers address the most common questions about gallbladder disease and cholecystectomy, including symptoms, indications for surgery, surgical strategy and recovery.
The following answers address the most common questions about gallbladder disease and cholecystectomy, including symptoms, indications for surgery, surgical strategy and recovery.
What is gallbladder disease?
Gallbladder disease refers to conditions affecting the gallbladder, most commonly gallstones, inflammation (cholecystitis) or gallbladder polyps. These conditions may cause pain, digestive symptoms or complications.
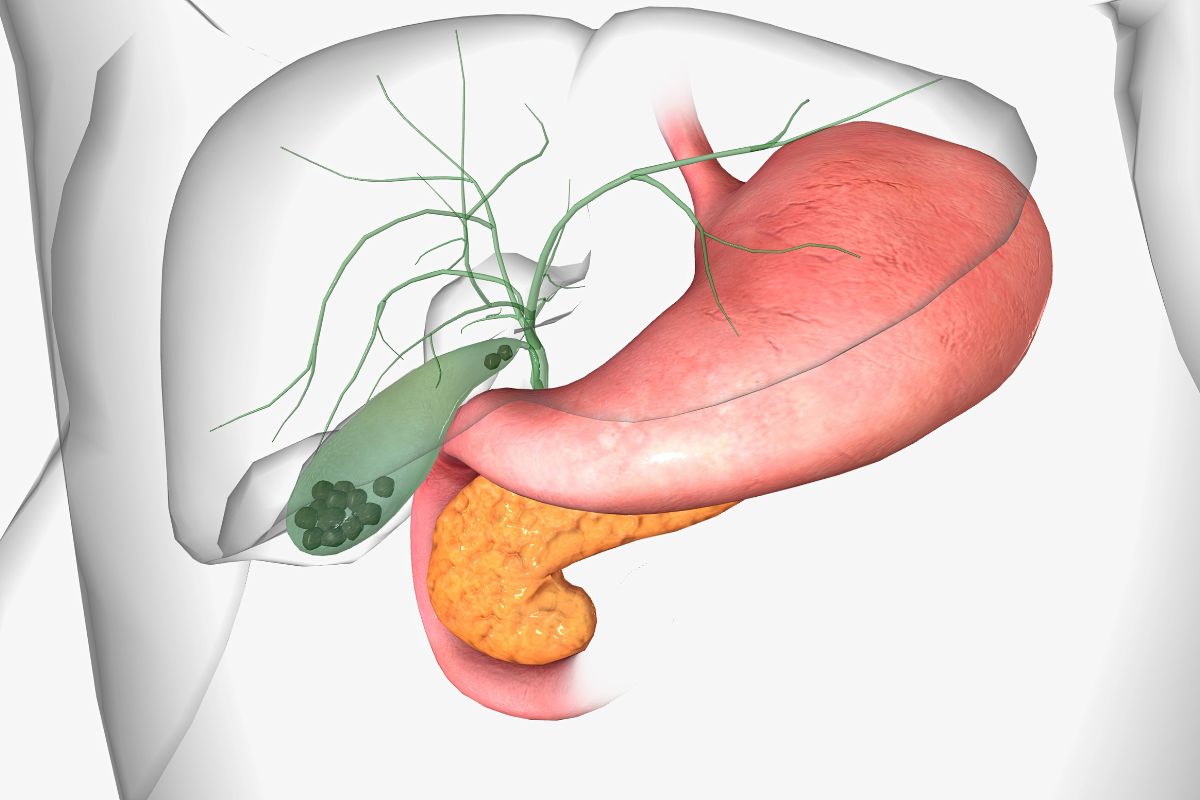
What are gallstones?
Gallstones are solid deposits that form inside the gallbladder from bile components. They may remain asymptomatic or cause biliary colic, inflammation or infection when they obstruct bile flow.
Do gallstones always require surgery?
No. Asymptomatic gallstones often do not require treatment. Surgery is considered when stones cause recurrent pain, inflammation or complications, or when the risk profile justifies intervention.
What are gallbladder polyps?
Gallbladder polyps are growths arising from the gallbladder wall. Most are benign, but some carry a risk of malignant transformation depending on size, appearance and patient factors. Surgery is usually recommended for polyps larger than 10 mm, rapidly growing lesions or polyps associated with symptoms or risk factors, as these may carry an increased cancer risk.
How is gallbladder disease treated surgically?
When indicated, treatment consists of cholecystectomy, the removal of the gallbladder. At Geneva Surgery, this is performed using a fully robotic approach with enhanced anatomical visualisation.
Why use robotic surgery for gallbladder disease?
Robotic surgery allows precise dissection within defined anatomical planes and improved identification of biliary structures using ICG fluorescence and intraoperative cholangiography, aiming the complication rate to the lowest possible.
Is gallbladder surgery safe in difficult situations?
Yes. With appropriate expertise and advanced imaging, robotic cholecystectomy offers a high level of safety, even in inflammatory or anatomically complex situations.
What is recovery like after gallbladder surgery?
Recovery is usually rapid. Patients are mobilised early, resume oral intake quickly and often return to normal daily activities within a short period.
Can you live normally without a gallbladder?
Yes. The gallbladder is not essential for digestion. Most patients have no long-term dietary limitations and experience normal digestive function after surgery.