Digestive Oncological Surgery
Digestive Oncological Surgery
ONCOLOGY
ONCOLOGY
The following answers address the most common questions related to digestive oncological surgery, including indications, decision-making and surgical management.
The following answers address the most common questions related to digestive oncological surgery, including indications, decision-making and surgical management.
What types of digestive cancers are treated at Geneva Surgery?
Geneva Surgery manages a broad spectrum of digestive oncological conditions. This includes colorectal cancers, small bowel malignancies, gastric cancer excluding tumours of the oesophagogastric junction, as well as selected neuroendocrine tumours, gastrointestinal stromal tumours and carcinoid tumours. Certain rare abdominal wall tumours, such as desmoid tumours, are also managed within a specialised framework.
How are decisions made in oncological surgery?
Management of digestive cancers is inherently multidisciplinary. Each case is discussed within appropriate tumour boards, bringing together surgical, medical oncology, gastroenterology, radiology, radio-oncology, nuclear medicine and medical genetics expertise when indicated. This ensures that surgery is integrated coherently into the overall oncological strategy.
What is the role of surgery in the oncological pathway?
Surgery represents one cardinal component of a global, coordinated oncological management plan. When surgical treatment is indicated, it is performed as a balanced expression of strict oncological principles and advanced reconstructive expertise, aligned with the broader therapeutic strategy.
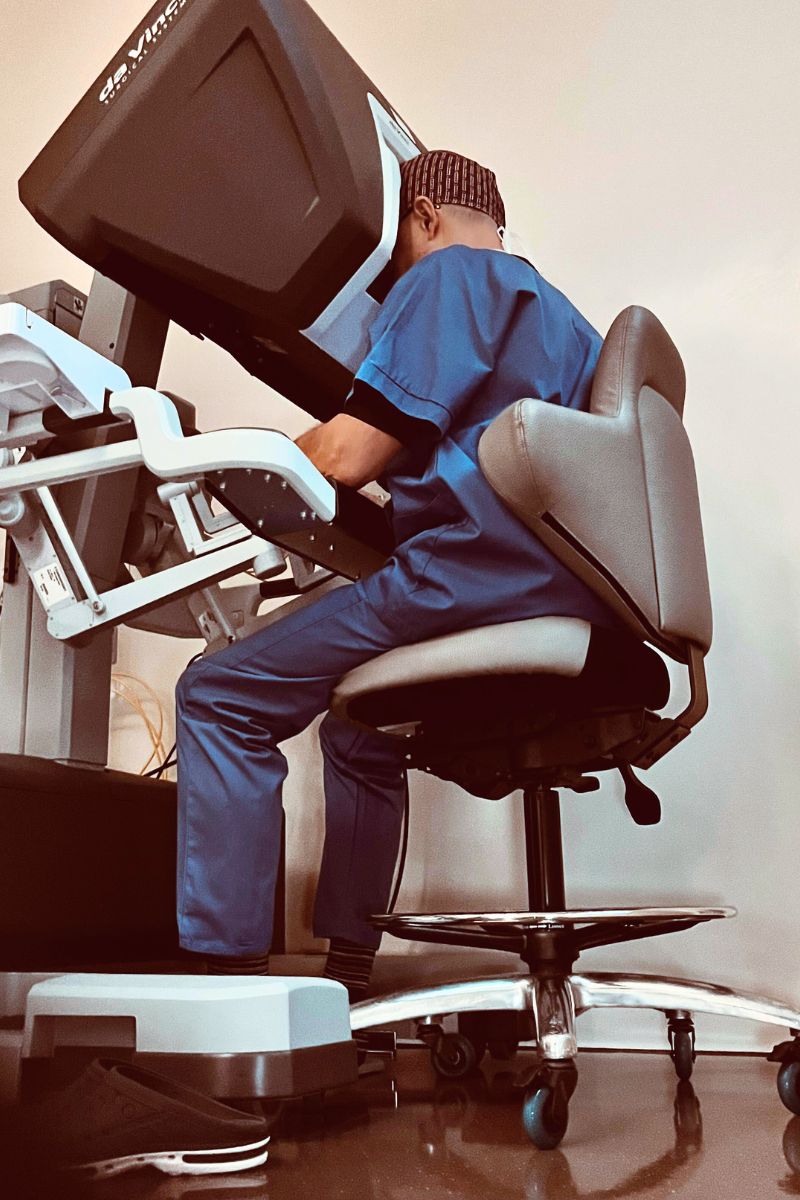
How does minimally invasive robotic surgery contribute in oncology?
Robotic surgery allows precise dissection and controlled reconstruction, particularly in anatomically constrained regions such as the pelvis or upper abdomen and in complex situations beyond the limits of standard laparoscopic approaches. This precision extends the scope of minimally invasive surgery, reduces conversion to open procedures and limits surgical trauma while maintaining oncological rigour.
What oncological principles guide surgical execution?
When surgery is indicated, procedures are planned and performed with strict respect for oncological principles, including appropriate resection margins and comprehensive lymphatic clearance. This level of precision supports consistent oncological execution and durable results.
Why is avoidance of complications a major objective in cancer surgery?
Beyond oncological rigour, a key objective of surgery is to achieve an uncomplicated postoperative course. This allows patients to return promptly to their oncological treatment plan, preserving continuity and coherence of the overall therapeutic strategy.
How are patients prepared and supported around oncological surgery?
Care pathways integrate multimodal prehabilitation, nutritional optimisation and systematic immunonutrition, aligned with ERAS principles. Opioid-free pain management strategies, physiotherapy focused on early and continued mobilisation, pulmonary exercises and close postoperative monitoring are standard components of care. Patients remain hospitalised until predefined recovery criteria are achieved, ensuring a safe and predictable transition to the next phase of treatment.
Is surgery sometimes performed in urgent oncological situations?
Yes. In certain situations, surgery may be required urgently to address complications related to cancer. In all cases, surgical intervention is considered within the context of the global oncological strategy and coordinated closely with the multidisciplinary team.
How are decisions made in oncological surgery?
Decisions are made within a structured multidisciplinary framework. Each case is discussed in tumour boards involving surgeons, medical oncologists, gastroenterologists, radiologists, pathologists, radio-oncologists, nuclear medicine specialists and medical genetics experts when appropriate. This ensures that surgical indications are based on a comprehensive analysis of the disease and integrated into a coherent, patient-specific oncological plan.
Is surgery performed independently or as part of a broader cancer strategy?
Surgery is never isolated from the overall oncological context. It is planned and performed as part of a coordinated treatment strategy discussed in tumour boards. This ensures continuity between surgical care, systemic treatments and long-term follow-up, with each step contributing to the global therapeutic objective.
What role does pathology play in oncological management?
Pathological analysis is a central element of oncological decision-making. Pathologists contribute to tumour board discussions, ensuring accurate diagnosis, staging and assessment of tumour characteristics. Their input is essential to guide surgical planning and to coordinate subsequent oncological treatments.