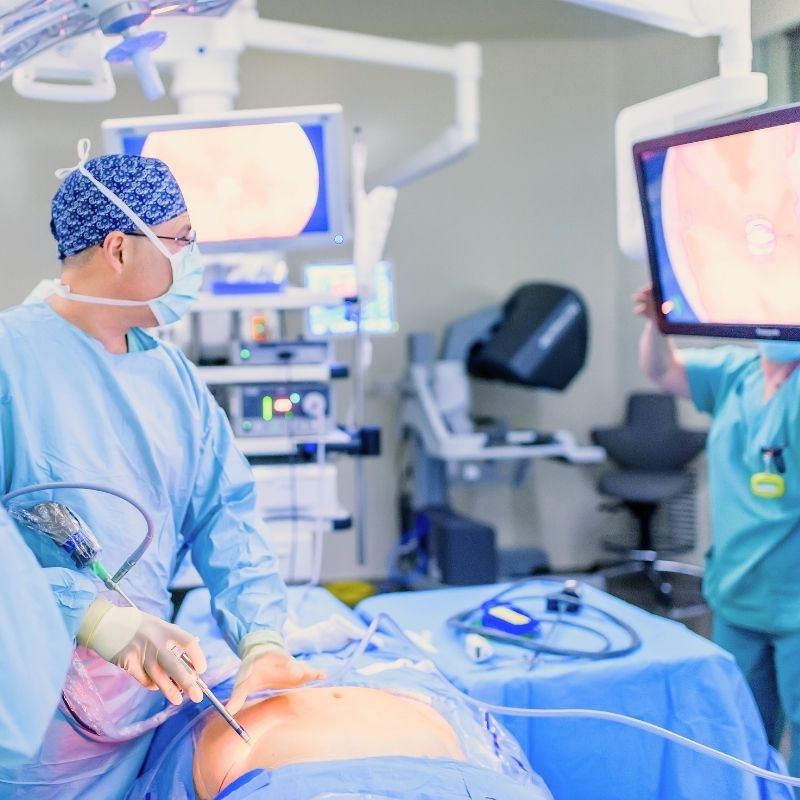
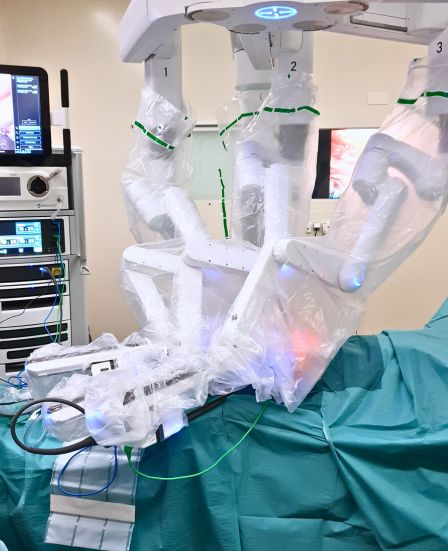
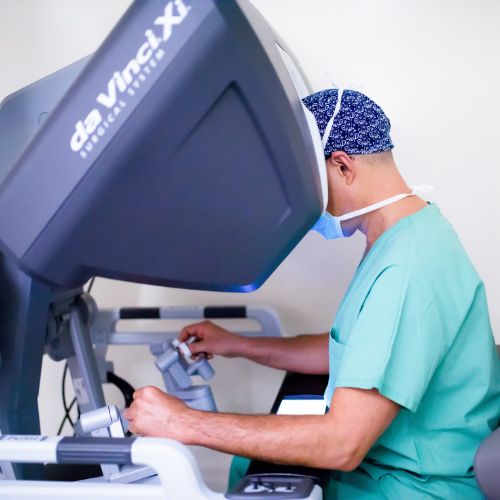
robotic visceral surgery Geneva
robotic visceral surgery Geneva
INGUINAL HERNIA
INGUINAL HERNIA
The following answers address the most common questions about inguinal hernia, including symptoms, indications for surgery and recovery.
The following answers address the most common questions about inguinal hernia, including symptoms, indications for surgery and recovery.
What symptoms can a inguinal hernia cause?
Groin hernias can present in different ways. Some patients notice a bulge, while others experience discomfort, pain, pressure or functional limitation. Symptoms often fluctuate and may be influenced by physical effort or posture. In some situations, groin pain may have another origin, which is why accurate diagnosis is essential.
Does every inguinal hernia require surgery?
Not necessarily. The indication for surgery depends on symptoms, impact on daily activities and, most importantly, the individual risk profile. Some hernias can be monitored safely, while others benefit from repair to improve function or reduce the risk of complications. The decision is approached as a risk management process, based on objective assessment and a clear discussion of available options.
Why is robotic surgery used for inguinal hernia repair?
Robotic surgery allows precise dissection and controlled reconstruction in a confined anatomical area. This level of precision supports accurate identification of anatomical planes, careful tissue handling and reliable reinforcement placement. The benefits of the robotic platform increase with the complexity of the situation, such as bilateral hernias, recurrent cases or anatomy altered by previous surgery. These principles are supported by clinical experience and recent scientific work in the field.
Can inguinal hernia surgery prevent future problems?
Yes. When indicated and performed appropriately, repair aims to restore abdominal wall integrity and reduce the risk of progression or complications. Long-term durability and functional outcome are central objectives of the surgical strategy.
How is recovery after inguinal hernia surgery?
Recovery is guided individually. Early mobilisation is encouraged, pain is managed with an opioid-free strategy and patients return progressively to normal activities according to recovery milestones discussed in advance.