GENEVA SURGERY
Geneva surgery
INCISIONAL HERNIA
INCISIONAL HERNIA
The following answers address the most common questions about incisional hernia, including symptoms, indications for surgery, preparation and recovery.
The following answers address the most common questions about incisional hernia, including symptoms, indications for surgery, preparation and recovery.
What is an incisional hernia?
An incisional hernia develops at the site of a previous surgical incision when healing of the abdominal wall is incomplete or progressively weakened. Unlike primary ventral hernias, incisional hernias result from prior surgical disruption of the abdominal wall anatomy and are associated with altered tissue quality. They often evolve over time and may increase in size or functional impact.
What symptoms can an incisional hernia cause?
Incisional hernias may present as a visible bulge, discomfort, pain or functional limitation. Symptoms can progress gradually and may interfere with posture, mobility or daily activities. Beyond local symptoms, incisional hernias can compromise abdominal wall function and core stability.
Does every incisional hernia require surgery?
Not necessarily. The indication for surgery depends on symptoms, functional impairment and individual risk profile. Some incisional hernias can be monitored safely, while others benefit from reconstruction to restore abdominal wall integrity and function. The decision is approached as a structured risk management process based on objective assessment.
Why are incisional hernias considered more complex?
Incisional hernias combine a structural defect with altered anatomy and reduced tissue quality due to previous surgery. Adhesions, scar tissue and muscle retraction increase technical complexity and influence reconstructive strategy. These factors require careful planning and tailored surgical execution.
What are the principles of incisional hernia repair at Geneva Surgery?
Repair follows modern reconstructive principles within a minimally invasive philosophy. The objectives are full anatomical restoration of the abdominal wall, wide extraperitoneal reinforcement for durability and functional reorganisation of the core. Avoidance of invasive fixation and minimisation of surgical trauma are central objectives. Functional restoration is prioritised over purely anatomical correction.
How are large or complex incisional hernias prepared?
Large or complex incisional hernias may require preoperative conditioning to optimise outcomes. Strategies such as abdominal wall preconditioning, including component separation techniques, progressive pneumoperitoneum or botulinum toxin when appropriate, are integrated within a structured multidisciplinary framework. The objective is to restore abdominal domain and facilitate safe reconstruction.
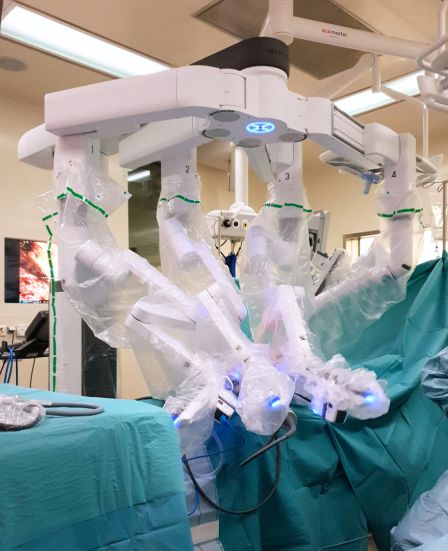
Why is robotic surgery used for incisional hernia repair?
Robotic surgery allows precise dissection in scarred and altered anatomical planes, controlled reconstruction and accurate placement of large extraperitoneal reinforcement. Its value increases with complexity and supports durable repair while limiting surgical trauma and conversion to open surgery.
How is recovery after incisional hernia surgery?
Recovery is structured and individualised. Pain management follows an opioid-free strategy, early mobilisation is encouraged and functional recovery is guided progressively. Patients remain hospitalised until predefined recovery criteria are achieved, ensuring a safe and predictable return to daily life.